At a glance
This report provides an update to the April 26, 2024, report to include three additional sporadic human cases (1 in Australia and 2 in the United States) and recent activity in wild birds, poultry, and other animals, including the multi-state outbreak in U.S. dairy cattle, and updated information on monitoring for human infections with highly pathogenic avian influenza A(H5N1) virus infections in the United States. CDC continues to believe that the overall risk to human health associated with the ongoing outbreaks of highly pathogenic avian influenza A(H5N1) viruses has not changed and remains low to the U.S. general public at this time.
Executive summary
A small number of sporadic human cases of highly pathogenic avian influenza (HPAI) A(H5N1) have been identified worldwide since 2022, amidst a panzootic of these viruses in wild birds and poultry. Nearly all human cases reported globally since 2022 were associated with poultry exposures, and no cases of human-to-human transmission of HPAI A(H5N1) virus have been identified. Three human cases of HPAI A(H5N1) virus infection in dairy farm workers were reported during April and May 2024 in the United States and were attributed to exposures to dairy cattle. One previous human case was detected in the United States in 2022 during poultry culling work. In a few cases, the source of exposure to HPAI A(H5N1) virus was unknown. To date, HPAI A(H5N1) viruses currently circulating most commonly in birds and poultry, with spillover to mammals and humans, do not have the ability to efficiently bind to receptors that predominate in the human upper respiratory tract. This is a major reason why the current risk to the public from HPAI A(H5N1) viruses remains low. However, because of the potential for influenza viruses to rapidly evolve and the wide global prevalence of HPAI A(H5N1) viruses in wild birds and poultry outbreaks and following the identification and spread among dairy cattle in the United States, additional sporadic human infections are anticipated. Continued comprehensive surveillance of these viruses in wild birds, poultry, mammals, and people worldwide, and frequent reassessments are critical to determine the public health risk, along with ongoing preparedness efforts.
Key findings
- CDC is actively working on the domestic outbreak of clade 2.3.4.4b HPAI A(H5N1) viruses in wild birds, with outbreaks in poultry and backyard flocks, and infections of other animals, including dairy cattle. Response activities include conducting surveillance among people with relevant exposures and preparing for the possibility that contemporary HPAI A(H5N1) viruses gain the ability for increased transmissibility to and among people.
- CDC, along with state and local public health partners, continues to monitor people in the United States who have been exposed to infected birds, poultry, dairy cattle, or other animals for 10 days after their last exposure. To date, more than 9,000 people in 52 jurisdictions have been monitored since 2022.
- H5 candidate vaccine viruses (CVVs) produced by CDC are expected to provide good protection against current clade 2.3.4.4b HPAI A(H5N1) viruses detected in birds and mammals, including dairy cattle. These H5 CVVs are available and have been shared with vaccine manufacturers.
- Because influenza viruses are constantly changing, CDC performs ongoing analyses of HPAI A(H5N1) viruses to identify genetic changes that might allow for: spread more easily to and between people, more serious illness in people, reduced susceptibility to antivirals, changes in the sensitivity of diagnostic assays, or reduced neutralization of the virus by vaccine induced antibodies. To date, few genetic changes of public health concern have been identified in HPAI A(H5N1) viruses circulating in wild birds and poultry worldwide and detected in dairy cattle in the United States.
- Currently, HPAI A(H5N1) viruses circulating in birds and U.S. dairy cattle are believed to pose a low risk to the general public in the United States; however, people who have job-related or recreational exposures to infected birds or mammals are at higher risk of infection and should take appropriate precautions outlined in CDC guidance.
- Comprehensive surveillance and readiness efforts are ongoing, and CDC continually takes preparedness measures to be ready in case the risk to people from HPAI A(H5N1) virus or from other novel influenza A viruses changes.
HPAI A(H5N1) viruses in wild birds and poultry
Since 2005, HPAI A(H5N1) viruses have undergone extensive genetic diversification including the formation of hundreds of genotypes following reassortment with other avian influenza A viruses. Clade 2.3.4.4b HPAI A(H5N1) viruses emerged in 2020 and were introduced into North America in late 2021 12 and spread to Central and South America, resulting in wild bird infections (in terrestrial, seabird, shorebird, and migratory species) and poultry outbreaks in many countries 345678. In Fall 2023, the first detections of HPAI A(H5N1) viruses in birds in the Antarctica region were reported 9. Globally, this 2.3.4.4b clade of HPAI A(H5N1) viruses has become widespread causing record numbers of bird outbreaks in wild, backyard, village, and farm birds.
In the United States, USDA APHIS monitors for avian influenza A viruses in wild, commercial, and backyard birds. From January 2022 through June 4, 2024, APHIS reported HPAI A(H5)/A(H5N1) virus detections in more than 9,300 wild birds in 50 states or territories and more than 1,140 commercial and backyard flocks affecting more than 96.5 million birds in 48 states.
HPAI A(H5N1) virus infections among mammals
Sporadic HPAI A(H5N1) virus infections of mammals have been reported since 2003-2004 during HPAI A(H5N1) virus outbreaks in poultry or wild birds 101112. HPAI A(H5) viruses are known to occasionally infect mammals that eat (presumably infected) birds or poultry and mammals that are exposed to environments with a high concentration of virus.
Globally, sporadic HPAI A(H5N1) virus infections and outbreaks in a wide range of mammal species were reported by countries in different regions of the world to the World Organisation for Animal Health since January 2022. HPAI A(H5N1) virus infections of mammals have included a polar bear in the United States, farmed mink in Spain and farmed foxes and other mammals in Finland, harbor and gray seals in the United States, sea lions in Peru, Argentina, and Chile, elephant seals in Argentina, baby goats in the United States, alpacas in the United States, and domesticated pets such as cats in Poland, France, South Korea, and the United States, and dogs in Italy. During March through June 4, 2024, the United States reported HPAI A(H5N1) virus infections of dairy cows at more than 80 farms in nine states. Spread from dairy farm-to-dairy farm was reported, and routes of transmission are under investigation. In the United States, from May 2022 through June 4, 2024, USDA APHIS reported HPAI A(H5N1) virus detections in wild mammals comprising a wide range of different species in 31 states.
Experimental studies have used the ferret model to assess transmissibility and disease severity of HPAI A(H5N1) clade 2.3.4.4b viruses. One study used a recombinant virus that was based upon a virus isolated from a mink during a mink farm outbreak in Spain in 2022. When ferrets were experimentally infected with the recombinant HPAI A(H5N1) clade 2.3.4.4b virus, transmission to co-housed susceptible ferrets through direct contact was observed, but transmission through respiratory droplets to separated ferrets was less efficient 13. In another study, ferrets experimentally infected with a HPAI A(H5N1) clade 2.3.4.4b virus isolated from a human case in Chile in 2023 transmitted to susceptible ferrets by direct contact but not through respiratory droplets or fomites 14. Importantly, in this study, all experimentally infected ferrets experienced fatal disease 14.
Human cases of A(H5N1)
While HPAI A(H5N1) viruses are currently circulating widely in wild birds and poultry in many geographic regions, relatively few human cases of HPAI A(H5N1) have been reported in recent years [Figure 1]. From January 2022 through June 4, 2024, 29 sporadic human cases of A(H5N1) were reported from nine countries, including 15 cases of severe or critical illness, and seven deaths, six cases of mild illness, and eight asymptomatic cases [Table 1].
One human case of HPAI A(H5N1) was reported in the United States in April 2022 while exposed to poultry. The individual reported fatigue without other symptoms during poultry culling activities at a farm with confirmed HPAI A(H5N1) virus infection of poultry, and a low level of A(H5N1) viral RNA was detected in a single upper respiratory tract specimen. It is possible that detection of A(H5N1) viral RNA resulted from deposition of non-infectious viral material in the upper respiratory tract of the individual and did not represent true infection, similar to the environmental contamination that was attributed to two asymptomatic cases in poultry workers reported in Spain 15. Transient environmental deposition may also explain the detection of A(H5N1) viral RNA in cases of A(H5N1) reported in asymptomatic poultry workers in the U.K. that were investigated as part of a surveillance study 161718.
One human case of A(H5N1) was reported in the United States in April 2024 in an adult dairy farm worker. The individual worked at a farm with sick cows presumed to be infected with HPAI A(H5N1) virus in an area in which cows at other dairy farms were confirmed with HPAI A(H5N1) virus infection in Texas 19. The worker only experienced conjunctivitis without any other signs or symptoms of illness. HPAI A(H5N1) virus was detected in conjunctival and nasopharyngeal swab specimens, and sequence data confirmed clade 2.3.4.4b, genotype B3.13, and close genetic relatedness to viruses detected in other dairy cattle farms in Texas. Oseltamivir was provided for treatment of the individual and for post-exposure prophylaxis of household contacts. Conjunctivitis resolved without other symptoms and household contacts remained well 19. No additional human cases related to this case were detected.
One human case of A(H5N1) was reported in the United States in May 2024 in an adult dairy farm worker. The individual worked at a farm with sick cows confirmed to be infected with HPAI A(H5N1) virus in Michigan. The worker only experienced conjunctivitis. HPAI A(H5N1) virus was detected in a conjunctival swab specimen, and sequence data confirmed clade 2.3.4.4b, genotype B3.13, closely related to genotype B3.13 viruses detected in dairy cows were sequenced and shared by USDA. Oseltamivir was offered to the worker and household contacts. No additional human cases related to this case were detected.
One human case of A(H5N1) was reported in the United States in May 2024 in an adult farm worker. The individual worked at a farm with sick cows confirmed to be infected with HPAI A(H5N1) virus in Michigan. The worker experienced upper respiratory symptoms. HPAI A(H5N1) virus was detected in a nasopharyngeal swab specimen, and partial HA and full-length NA sequence data confirmed clade 2.3.4.4b, closely related to viruses detected in dairy cows. Oseltamivir was provided for treatment of the individual and for post-exposure prophylaxis of household contacts. No additional human cases related to this case were detected.
Most human cases of HPAI A(H5N1) reported since January 2022 had recent exposure to sick or dead poultry, and no cases of human-to-human HPAI A(H5N1) virus transmission were identified. Fifteen cases (8 children, 7 adults) had severe or critical illness, and seven (3 children, 4 adults) died. Fifteen cases were associated with clade 2.3.4.4b HPAI A(H5N1) virus in six countries, and 12 cases were associated or assumed to be associated with clade 2.3.2.1c HPAI A(H5N1) viruses in Cambodia and Vietnam. Of the seven cases of clade 2.3.4.4b HPAI A(H5N1) virus infection with conjunctivitis or respiratory illness (excludes one case with fatigue only), four had severe or critical illness (57%), and 1 of the 4 died (25%). One case of severe illness in a child in Australia in March 2024 with recent travel history to India was associated with clade 2.3.2.1a HPAI A(H5N1) virus. None of the HPAI A(H5N1) virus genetic sequences contained any known markers of reduced susceptibility to currently recommended FDA-approved influenza antiviral medications.
Genetic data have revealed that when some mammals, including humans, are infected with HPAI A(H5N1) virus, the virus may undergo intra-host evolution resulting in genetic changes that allow more efficient replication in the lower respiratory tract or extrapulmonary tissues 202122. Some HPAI A(H5N1) viruses that have infected humans in 2023 and 2024 have also shown the same or similar genetic changes as those identified in wild and captive mammals. For example, sequencing of viruses from specimens collected from human cases identified in Cambodia during October and November 2023, in Vietnam in 2024 and in the dairy farm worker in Texas in April 2024 revealed the presence of the polymerase basic protein 2 (PB2) 627K marker, which is often associated with mammalian adaptation during infection 23. The HPAI A(H5N1) virus sequenced from the human case in Chile identified in March 2023 had different genetic changes (PB2 591K and 701N) that are also associated with mammalian adaptation 24. Sequencing of the HPAI A(H5N1) virus from the first dairy farm worker case in Michigan did not identify the PB2 627K marker but revealed the presence of PB2 M631L, that is known to be associated with viral adaptation to mammalian hosts, and which has been detected in 99% of dairy cow sequences but only sporadically in birds 25. PB2 M631L has been identified as resulting in enhancement of virus replication and disease severity in mice during studies with avian influenza A(H10N7) viruses 26. The remainder of the genome of A/Michigan/90/2024 was closely related to sequences detected in infected dairy cows and strongly suggests cow-to-human transmission.
Although these genetic changes may impact mammalian disease outcome, they have not been associated with enhanced transmissibility of the virus to humans. HPAI A(H5N1) viruses preferentially bind to α2,3-linked sialic acid receptors that are prevalent in the respiratory and intestinal tracts of waterfowl and poultry, and in the human lower respiratory tract but do not currently have the ability to easily infect cells and bind efficiently to α2,6-linked sialic acid receptors that are predominant in the human upper respiratory tract 2. The ability to bind efficiently to α2,6-linked sialic acid receptors would be needed to increase the risk of transmission to people 2728. Using recombinantly expressed hemagglutinin, analysis of receptor binding of the HPAI A(H5N1) virus identified in the dairy farm worker from Texas (A/Texas/27/2024) revealed binding only to avian-type α2,3-linked sialic acid receptors.
Table 1. Global reported A(H5N1) human cases, January 2022 through June 4, 2024
| Country of Case | Month of illness onset or case detection | Disease Severity and Outcome | Virus Clade by sequencing or associated poultry outbreaks |
|---|---|---|---|
| Australia (after travel to India) | March 2024 | Severe illness, survived | Clade 2.3.2.1a |
| Cambodia | February 2023 | Critical illness, died | Clade 2.3.2.1c |
| February 2023 | Mild illness | Clade 2.3.2.1c | |
| October 2023 | Critical illness, died | Clade 2.3.2.1c | |
| October 2023 | Critical illness, died | Clade 2.3.2.1c | |
| November 2023 | Critical illness, died | Clade 2.3.2.1c | |
| November 2023 | Mild illness | Clade 2.3.2.1c | |
| January 2024 | Severe illness, survived | Clade 2.3.2.1c | |
| January 2024 | Severe illness, survived | Clade 2.3.2.1c | |
| January 2024 | Critical illness, died | Clade 2.3.2.1c | |
| February 2024 | Severe illness, survived | Not reported | |
| February 2024 | Asymptomatic | Clade 2.3.2.1c | |
| Chile | March 2023 | Critical illness, survived | Clade 2.3.4.4b |
| China | September 2022 | Critical illness, died | Clade 2.3.4.4b |
| January 2023 | Severe illness, outcome not reported | Clade 2.3.4.4b | |
| Ecuador | December 2022 | Critical illness, survived | Clade 2.3.4.4b |
| Spain | September 2022 | Asymptomatic | Clade 2.3.4.4b |
| October 2022 | Asymptomatic | Clade 2.3.4.4b | |
| United Kingdom | January 2022 | Asymptomatic | Clade 2.3.4.4b |
| May 2023 | Asymptomatic | Clade 2.3.4.4b | |
| May 2023 | Asymptomatic | Clade 2.3.4.4b | |
| July 2023 | Asymptomatic | Clade 2.3.4.4b | |
| July 2023 | Asymptomatic | Clade 2.3.4.4b | |
| United States | April 2022 | Mild illness (fatigue) | Clade 2.3.4.4b |
| March 2024 | Mild illness (conjunctivitis) | Clade 2.3.4.4b | |
| May 2024 | Mild illness (conjunctivitis) | Clade 2.3.4.4b | |
| May 2024 | Mild illness | Clade 2.3.4.4b | |
| Vietnam | October 2022 | Critical illness, survived | Not reported |
| March 2024 | Critical illness, died | Clade 2.3.2.1c |
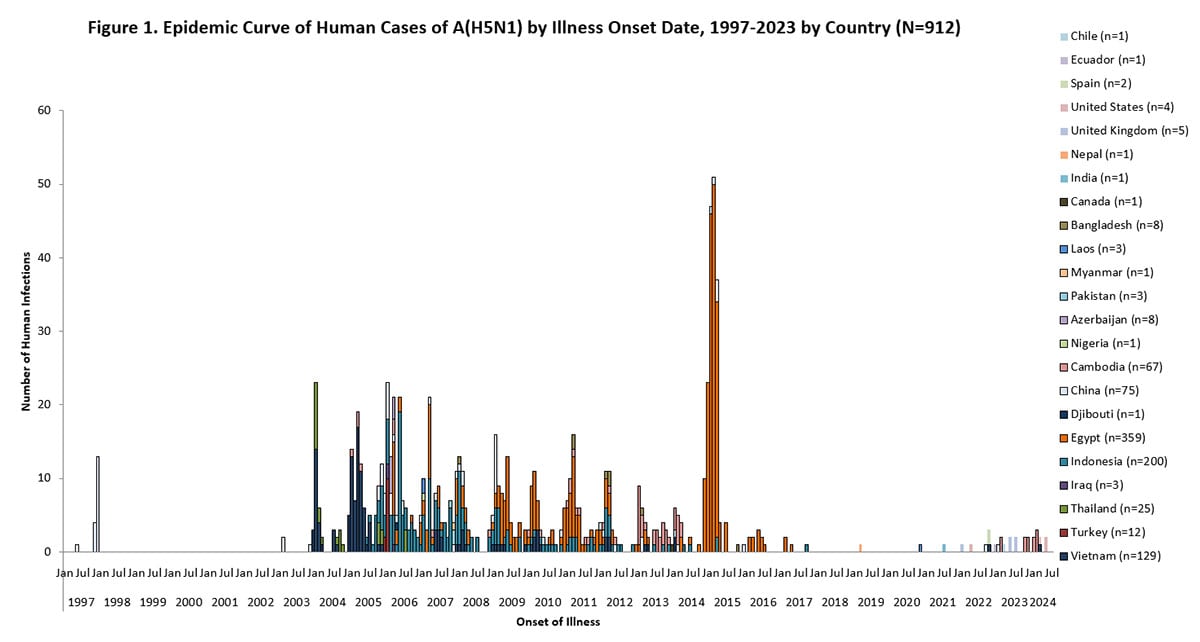
Since 1997, a total of 912 sporadic human A(H5N1) cases have been reported from 24 countries, caused by different HPAI A(H5N1) virus clades [29,30], with a cumulative case fatality proportion of greater than 50%. Human A(H5N1) cases peaked in 2006 (115 cases, 9 countries) and 2015 (145 cases, 4 countries) primarily due to a large epidemic in Egypt with 136 cases [Figure 1].
Nearly all reported human A(H5N1) cases had poultry exposures, such as to sick or dead poultry or visiting live poultry markets. Rare, limited, and non-sustained instances of human-to-human HPAI A(H5N1) virus transmission likely occurred in a small number of family members following prolonged, close unprotected exposure with a symptomatic case-patient during 2004-2007 in multiple countries 29303132.
Figure 1. Epidemic Curve of Human Cases of A(H5N1) by Illness Onset Date, 1997-2024 by Country (N=912)
Monitoring of persons exposed to HPAI A(H5N1) viruses in the United States
Although few human cases have occurred recently, given widespread infection among poultry and wild birds, people who have job-related or recreational exposures to infected birds or sick or dead mammals are at higher risk of infection.
CDC, in collaboration with state, territorial, and local public health partners, has monitored people exposed to infected birds and poultry, cattle, or other animals beginning with their first exposure and for 10 days after their last exposure, from February 2022 through June 4, 2024:
- Total monitored: more than 9,000 people in 52 jurisdictions.
- Total illnesses reported among monitored persons: nearly 200 people.
- Number positive for influenza A(H5N1) virus: 3 people (1 additional case was detected in a dairy farm worker not being monitored).
Of the nearly 200 monitored people showing symptoms who were tested for novel influenza A and seasonal influenza viruses along with other respiratory viruses, HPAI A(H5N1) virus was detected in specimens from 3 persons. HPAI A(H5N1) virus genetic material was detected at a low level in a respiratory specimen from one person in Colorado who experienced fatigue without any other illness signs or symptoms while participating in poultry culling activities. HPAI A(H5N1) virus was detected in a conjunctival swab specimen from one person in Michigan who experienced conjunctivitis without any other illness signs or symptoms while working with sick dairy cattle confirmed with HPAI A(H5N1) virus infection. HPAI A(H5N1) virus genetic material was detected in a nasopharyngeal swab specimen from one person in Michigan who experienced acute respiratory illness while working with sick dairy cattle confirmed with HPAI A(H5N1) virus infection. HPAI A(H5N1) virus was detected in conjunctival swab and nasopharyngeal swab specimens in one person in Texas who was not being monitored who experienced conjunctivitis without any other illness signs or symptoms while working with sick dairy cattle presumed to be infected with HPAI A(H5N1) virus. [See above section on "Human cases of A(H5N1)."]
U.S. influenza surveillance for human infections with novel influenza A viruses, including HPAI A(H5N1) virus
Human infection with a novel influenza A virus, including HPAI A(H5N1) virus, is a nationally notifiable condition (case definition: Novel Influenza A Virus Infections 2014 Case Definition | CDC)
Influenza testing is widely available in clinical laboratories and health care facilities. Assays in these settings would detect A(H5N1) virus infections as influenza A virus positive, and a subset of assays would be able to also determine that they are not influenza A virus subtypes H1 or H3 that commonly circulate among humans. Specimens from persons possibly exposed to HPAI A(H5N1) virus or that test positive for influenza A virus but negative for A(H1) and A(H3) subtypes should be forwarded to the appropriate state or local public health laboratory for further testing. CDC should be notified immediately in the event that any clinical specimens from suspected cases test positive for a novel influenza A virus or if the testing results of clinical specimens from suspected cases are inconclusive. Currently, CDC recommends testing for HPAI A(H5N1) virus infection in symptomatic persons with relevant exposure history. Human infection with a novel influenza A virus is a nationally notifiable condition, and currently confirmatory testing is being done only at CDC. Very few specimens have been submitted to CDC for H5 testing since January 2022.
- Seasonal influenza virus detection assays that can also detect novel influenza A viruses are used in 128 public health laboratories in all 50 U.S states.
- Specific diagnostic assays to detect A(H5) viruses are available at 99 public health laboratories in all 50 states.
Per long-standing protocols, upon detection of a virus that tests positive for influenza A virus but is negative for human H1 or H3 genes, the public health laboratory will rapidly contact CDC and ship the specimen to CDC. Specimens that are influenza A virus positive but negative for human H1 or H3 genes may also be tested for H5 by state public health laboratories and are rapidly sent to CDC for a diagnostic result. An investigation of the case will be initiated, and a case report form will be submitted to CDC through the novel influenza A reporting module.
CDC and U.S. Government Preparedness Activities
Activity
Summary
Global surveillance and rapid response to human infections
CDC’s Influenza Division supports surveillance in live bird markets, backyard farms, and wild birds and/or their environments in Bangladesh, Cambodia, China, Guatemala, Kenya, Lao PDR, Peru, Thailand, and Vietnam. Surveillance data highlight the high prevalence and wide range of avian influenza A viruses in birds and help to describe the changing epidemiology of avian influenza A viruses. In 2022, the Influenza Division tracked more than 50 human infections with avian influenza A viruses reported to the WHO from seven countries in four WHO regions. Most recently, CDC Influenza Division field staff assisted in the rapid response investigations of four human A(H5N1) cases in Cambodia during October and November 2023.
- Influenza virus and illness activity are monitored year-round through a collaborative effort between CDC and many partners, including state, local, and territorial health departments; public health and clinical laboratories; clinics; and emergency departments.
- Human cases of novel influenza A virus infection, which are human infections with non-human influenza A viruses that are different from currently spreading seasonal human influenza A viruses, are nationally notifiable. Every identified case is investigated and reported to CDC.
- CDC is actively looking at multiple influenza indicators during the current situation to monitor for HPAI A(H5N1) viruses, including looking for spread of the virus to, or among people, in jurisdictions where the virus has been identified in people or animals.
Virological assessments
Because influenza viruses have a high error rate during replication and rapidly evolve, CDC continually conducts genetic analyses of viruses to identify changes that may impact virus phenotypes such as antigenicity, antiviral susceptibility, transmissibility, and/or pathogenesis. Genetic analysis also is performed to assess changes that may impact diagnostic test performance.
Diagnostics
Various CDC influenza virus diagnostic real time RT-PCR tests detect typical human (seasonal) viruses or novel influenza A viruses (e.g., H5, H7) that may infect people through zoonotic transmission. These diagnostic tests are used in all 50 U.S states and globally. Additionally, there are CDC diagnostic tests that specifically detect A(H5) viruses, which are available in public health laboratories in all 50 U.S. states and international laboratories.
Most commercial assays used for human influenza virus testing are likely to detect HPAI A(H5N1) viruses as influenza A viruses because they target conserved proteins.
Candidate vaccine virus development
The development of influenza candidate vaccine viruses (CVVs), coordinated by WHO, remains an essential component of the overall global strategy for influenza pandemic preparedness. A library of H5 candidate vaccine viruses (CVV) has been produced with additional recommendations for development during bi-annual vaccine consultation meetings (See Table and https://www.who.int/teams/global-influenza-programme/vaccines/who-recommendations/zoonotic-influenza-viruses-and-candidate-vaccine-viruses). The CDC Influenza Risk Assessment Tool is also used to help prioritize HPAI A(H5) viruses for development of CVVs.
Limitations of the Report
This report is subject to the following limitations. First, the number of reported human infections with HPAI A(H5N1) viruses is small. Conclusions regarding virus characterization analyses, transmissibility from animals to people, transmissibility among people, and clinical spectrum of illness in people should be interpreted in light of this small number. Second, detailed exposure information was not available for all exposed persons or for those being monitored for illness after exposure to HPAI A(H5N1) virus-infected wild birds, poultry, backyard flocks, and other animals, including dairy cattle in the United States. As of the date of this report, understanding of HPAI A(H5N1) virus infections of cattle is very limited. Thus, we are not able to assess the impact of exposure variables such as duration of exposure, nature of exposure (e.g., direct vs. indirect contact), and use of personal protective equipment on infection risk among persons with confirmed HPAI A(H5N1) virus infection or those being monitored after exposures to any animals confirmed or suspected with HPAI A(H5N1) virus infection.
Conclusions
- To date, CDC analyses of clade 2.3.4.4b HPAI A(H5N1) viruses detected in wild birds, poultry, and sporadically in mammals, including in dairy cattle, since late 2021 indicate that these viruses all have a high degree of genetic identity with each other and no significant mammalian adaptive substitutions, insertions, or deletions have been identified, particularly in the HA gene, which is important for zoonotic and subsequent human-to-human transmission.
- Considering the high prevalence of HPAI A(H5N1) viruses in wild birds and poultry worldwide, spillover into mammals (including carnivores that may feed on infected animals) and additional sporadic zoonotic infections are anticipated among people with exposures to infected sick or dead poultry, wild birds, or other infected animals.
- Clade 2.3.4.4b HPAI A(H5N1) viruses currently circulating in wild birds and poultry worldwide lack the ability to preferentially bind to the types of sialic acid receptors that are predominant in the upper respiratory tract of humans and therefore do not currently have the ability to easily infect or transmit among people.
- Despite extensive worldwide spread of HPAI A(H5N1) viruses in wild birds and poultry in recent years, only a small number of sporadic human infections with clade 2.3.4.4b or clade 2.3.2.1c viruses have been reported since 2022; nearly all cases had recent exposure to poultry and no cases of human-to-human transmission of HPAI A(H5N1) virus have been identified.
- In 2024, 3 sporadic epidemiologically unrelated human infections with clade 2.3.4.4b HPAI A(H5N1) viruses have been detected in U.S. dairy farm workers exposed to cows presumed or confirmed to be infected with HPAI A(H5N1) virus. All 3 workers experienced clinically mild illnesses and recovered fully. For cases with genome sequencing available, no known markers of reduced susceptibility to currently recommended FDA-approved influenza antiviral medications were detected, and no changes to receptor binding tropism were identified that would increase the risk of transmission to and among people. Given the ongoing outbreak of clade 2.3.4.4b HPAI A(H5N1) viruses among dairy cattle in 9 states to date, additional sporadic human infections in exposed dairy farm workers are anticipated.
While CDC's assessment is that the current overall threat of clade 2.3.4.4b HPAI A(H5N1) viruses to public health is low, the widespread geographic prevalence of infected birds and poultry, with spillover into a wide range of mammal species, and ongoing spread of clade 2.3.4.4b viruses, including among dairy cattle in the United States, raises the potential for more mammals to be infected that could result in viral evolution or reassortment events which might change the current risk assessment. Similar to human infections with HPAI A(H5N1) viruses since 1997, sporadic clade 2.3.4.4b HPAI A(H5N1) virus infections have resulted in a wide clinical spectrum, ranging from conjunctivitis and acute respiratory illness to severe and critical illness with fatal outcome. Additional sporadic human infections with HPAI A(H5N1) viruses with a wide clinical spectrum (mild to severe and critical illness) resulting from exposure to infected animals are anticipated worldwide. Vigilance and ongoing surveillance of HPAI A(H5N1) viruses circulating in wild birds, poultry, and in mammals and infected persons worldwide is critical to monitor the public health risk and to detect genetic changes (particularly in the HA gene) that would change CDC's risk assessment.
Resources
Previous H5N1 Technical Reports
Additional Information
References to non-CDC sites are provided as a service and do not constitute or imply endorsement of these organizations or their programs by CDC or the U.S. Department of Health and Human Services. CDC is not responsible for the content of pages found at these sites. URL addresses listed were current as of the date of publication.
- Bevins SN, Shriner SA, Cumbee JC Jr, Dilione KE, Douglass KE, Ellis JW et al. Intercontinental Movement of Highly Pathogenic Avian Influenza A(H5N1) Clade 2.3.4.4 Virus to the United States, 2021. Emerg Infect Dis. 2022 May;28(5):1006-1011.
- Kandeil A, Patton C, Jones JC, Jeevan T, Harrington WN, Trifkovic S et al. Rapid evolution of A(H5N1) influenza viruses after intercontinental spread to North America. Nat Commun. 2023 May 29;14(1):3082.
- World Health Organization. Antigenic and genetic characteristics of zoonotic influenza A viruses and development of candidate vaccine viruses for pandemic preparedness. February 2023. https://cdn.who.int/media/docs/default-source/influenza/who-influenza-recommendations/vcm-northern-hemisphere-recommendation-2023-2024/20230224_zoonotic_recommendations.pdf?sfvrsn=38c739fa_4
- European Food Safety Authority, European Centre for Disease Prevention and Control, European Union Reference Laboratory for Avian Influenza. Avian influenza overview March – April 2023. EFSA J 2023 Jun 7;21(6):e08039.
- Ariyama N, Pardo-Roa C, Muñoz G, Aguayo C, Ávila C, Mathieu C, Almonacid LI, Medina RA, Brito B, Johow M, Neira V. Highly Pathogenic Avian Influenza A(H5N1) Clade 2.3.4.4b Virus in Wild Birds, Chile. Emerg Infect Dis. 2023 Sep;29(9):1842-1845. Doi: 10.3201/eid2909.230067. Epub 2023 Jul 24. PMID: 37487166; PMCID: PMC10461661
- Leguia M, Garcia-Glaessner A, Muñoz-Saavedra B, Juarez D, Barrera P, Calvo-Mac C, Jara J, Silva W, Ploog K, Amaro L, Colchao-Claux P, Johnson CK, Uhart MM, Nelson MI, Lescano J. Highly pathogenic avian influenza A (H5N1) in marine mammals and seabirds in Peru. Nat Commun. 2023 Sep 7;14(1):5489. Doi: 10.1038/s41467-023-41182-0. PMID: 37679333; PMCID: PMC10484921.
- Pan American Health Organization. Epidemiological Update Outbreaks of avian influenza caused by influenza A(H5N1) in the Region of the Americas. 9 August 2023. https://www.paho.org/en/documents/epidemiological-update-outbreaks-avian-influenza-caused-influenza-ah5n1-region-americas-0
- Global Avian Influenza Viruses with Zoonotic Potential situation update, 28 March 2024. https://www.fao.org/animal-health/situation-updates/global-aiv-with-zoonotic-potential/en
- World Organisation for Animal Health. Wildlife under threat as avian influenza reaches Antarctica. 13 March 2024. https://www.woah.org/en/wildlife-under-threat-as-avian-influenza-reaches-antarctica/
- Keawcharoen J, Oraveerakul K, Kuiken T, Fouchier RAM, Amonsin A, Payungporn S et al. Avian influenza H5N1 in tigers and leopards. Emerg Infect Dis. 2004 Dec;10(12):2189-91.
- Songserm T, Amonsin A, Jam-on R, Sae-Heng N, Pariyothorn N, Payungporn S et al. Fatal avian influenza A H5N1 in a dog. Emerg Infect Dis. 2006 Nov;12(11):1744-7.
- Songserm T, Amonsin A, Jam-on R, Sae-Heng N, Meemak N, Pariyothorn N et al. Avian influenza H5N1 in naturally infected domestic cat. Emerg Infect Dis. 2006 Apr;12(4):681-3.
- Restori KH, Septer KM, Field CJ, Patel DR, VanInsberghe D, Raghunathan V, Lowen AC, Sutton TC. Risk assessment of a highly pathogenic H5N1 influenza virus from mink. Nat Commun. 2024 May 15;15(1):4112. doi: 10.1038/s41467-024-48475-y. https://pubmed.ncbi.nlm.nih.gov/38750016/
- Pulit-Penaloza JA, Brock N, Belser JA, Sun X, Pappas C, Kieran TJ, Thakur PB, Zeng H, Cui D, Frederick J, Fasce R, Tumpey TM, Maines TR. Highly pathogenic avian influenza A(H5N1) virus of clade 2.3.4.4b isolated from a human case in Chile causes fatal disease and transmits between co-housed ferrets. Emerg Microbes Infect. 2024 Mar 17:2332667. doi: 10.1080/22221751.2024.2332667. Online ahead of print. https://pubmed.ncbi.nlm.nih.gov/38494746/
- Aznar E, Casas I, González Praetorius A, Ruano Ramos MJ, Pozo F, Sierra Moros MJ et al.Influenza A(H5N1) detection in two asymptomatic poultry farm workers in Spain, September to October 2022: suspected environmental contamination. Euro Surveill. 2023 Feb;28(8):2300107. Doi: 10.2807/1560-7917.ES.2023.28.8.2300107. https://pubmed.ncbi.nlm.nih.gov/36820643/
- World Health Organization. Avian Influenza A(H5N1) – United Kingdom of Great Britain and Northern Ireland. 30 May 2023. Accessed at: https://www.who.int/emergencies/disease-outbreak-news/item/2023-DON468
- Capelastegui F, Smith J, Kumbang J, Humphreys C, Padfield S, Turner J et al. Pilot of asymptomatic swabbing of humans following exposures to confirmed avian influenza A(H5) in avian species in England, 2021/2022. Influenza Other Respir Viruses. 2023 Aug 23;17(8):e13187. Doi: 10.1111/irv.13187 https://pubmed.ncbi.nlm.nih.gov/37638093/
- UK Health Security Agency. Investigation into the risk to human health of avian influenza (influenza A H5N1) in England: technical briefing 5. Updated 14 July 2023. Accessed at: Investigation into the risk to human health of avian influenza (influenza A H5N1) in England: technical briefing 5 – GOV.UK (www.gov.uk)
- Uyeki TM, Milton S, Abdul Hamid C, Reinoso Webb C, Presley SM, Shetty V, Rollo SN, Martinez DL, Rai S, Gonzales ER, Kniss KL, Jang Y, Frederick JC, De La Cruz JA, Liddell J, Di H, Kirby MK, Barnes JR, Davis CT. Highly Pathogenic Avian Influenza A(H5N1) Virus Infection in a Dairy Farm Worker. N Engl J Med. 2024 May 3. doi: 10.1056/NEJMc2405371. Online ahead of print.
- Gabriel G, Czudai-Matwich V, Klenk HD. Adaptive mutations in the H5N1 polymerase complex. Virus Res. 2013 Dec 5;178(1):53-62. Doi: 10.1016/j.virusres.2013.05.010.
- Bogs J, Kalthoff D, Veits J, Pavlova S, Schwemmle M, Mänz B et al. Reversion of PB2-627E to -627K during replication of an H5N1 Clade 2.2 virus in mammalian hosts depends on the origin of the nucleoprotein. J Virol. 2011 Oct;85(20):10691-8. Doi: 10.1128/JVI.00786-11.
- Agüero M, Monne I, Sánchez A, Zecchin B, Fusaro A, Ruano MJ et al. Highly pathogenic avian influenza A(H5N1) virus infection in farmed minks, Spain, October 2022. Euro Surveill. 2023 Jan;28(3):2300001. Doi: 10.2807/1560-7917.ES.2023.28.3.2300001.
- CDC. Technical Update: Summary Analysis of Genetic Sequences of Highly Pathogenic Avian Influenza A(H5N1) Viruses in Texas. April 2, 2024. Accessed at: https://www.cdc.gov/bird-flu/spotlights/h5n1-analysis-texas.html
- CDC. Human Infection with highly pathogenic avian influenza A(H5N1) virus in Chile. Accessed at: https://www.cdc.gov/bird-flu/spotlights/chile-first-case-h5n1-addendum.html
- Nguyen TQ, Hutter C, Markin A, Thomas M, Lantz K, Killian ML, Janzen GM, Vijendran S, Wagle S, Inderski B, Magstadt DR, Li G, Diel DG, Frye EA, Dimitrov KM, Swinford AK, Thompson AC, Snevik KR, Suarez DL, Spackman E, Lakin SM, Ahola SC, Johnson KR, Baker AL, Robbe-Austerman S, Torchetti MK, Anderson TK. Emergence and interstate spread of highly pathogenic avian influenza A(H5N1) in dairy cattle bioRxiv 2024.05.01.591751; doi: https://doi.org/10.1101/2024.05.01.591751
- Zhang X, Xu G, Wang C, Jiang M, Gao W, Wang M, Sun H, Sun Y, Chang KC, Liu J, Pu J. Enhanced pathogenicity and neurotropism of mouse-adapted H10N7 influenza virus are mediated by novel PB2 and NA mutations. J Gen Virol. 2017 Jun;98(6):1185-1195. doi: 10.1099/jgv.0.000770. Epub 2017 Jun 8. PMID: 28597818.
- Van Riel D, den Bakker MA, Leijten LM, Chutinimitkul S, Munster VJ, de Wit E et al. Seasonal and pandemic human influenza viruses attach better to human upper respiratory tract epithelium than avian influenza viruses. Am J Pathol. 2010 Apr;176(4):1614-8. Doi: 10.2353/ajpath.2010.090949.
- Shinya K, Ebina M, Yamada S, Ono M, Kasai N, Kawaoka Y. Avian flu: influenza virus receptors in the human airway. Nature. 2006 Mar 23;440(7083):435-6. Doi: 10.1038/440435a.
- Ungchusak K, Auewarakul P, Dowell SF, Kitphati R, Auwanit W, Puthavathana P et al. Probable person-to-person transmission of avian influenza A (H5N1). N Engl J Med. 2005 Jan 27;352(4):333-40. Doi: 10.1056/NEJMoa044021. https://pubmed.ncbi.nlm.nih.gov/15668219/
- Wang H, Feng Z, Shu Y, Yu H, Zhou L, Zu R et al. Probable limited person-to-person transmission of highly pathogenic avian influenza A (H5N1) virus in China. Lancet. 2008 Apr 26;371(9622):1427-34. Doi: 10.1016/S0140-6736(08)60493-6. https://pubmed.ncbi.nlm.nih.gov/18400288/
- WHO Disease Outbreak News. 2006 – Indonesia. 31 May 2006. Accessed at: https://www.who.int/emergencies/disease-outbreak-news/item/2006_05_31-en
- World Health Organization. Human cases of avian influenza A (H5N1) in North-West Frontier Province, Pakistan, October-November 2007. Wkly Epidemiol Rec. 2008 Oct 3;83(40):359-64.
- Lai S, Qin Y, Cowling BJ, Ren X, Wardrop NA, Gilbert M et al. Global epidemiology of avian influenza A H5N1 virus infection in humans, 1997-2015: a systematic review of individual case data. Lancet Infect Dis. 2016 Jul;16(7):e108-e118. Doi: 10.1016/S1473-3099(16)00153-5. https://pubmed.ncbi.nlm.nih.gov/27211899/
- World Health Organization. Cumulative number of confirmed human cases for avian influenza A(H5N1) reported to WHO, 2003-2024, 3 May 2024. Accessed at: https://www.who.int/publications/m/item/cumulative-number-of-confirmed-human-cases-for-avian-influenza-a(h5n1)-reported-to-who–2003-2024-3-may-2024
